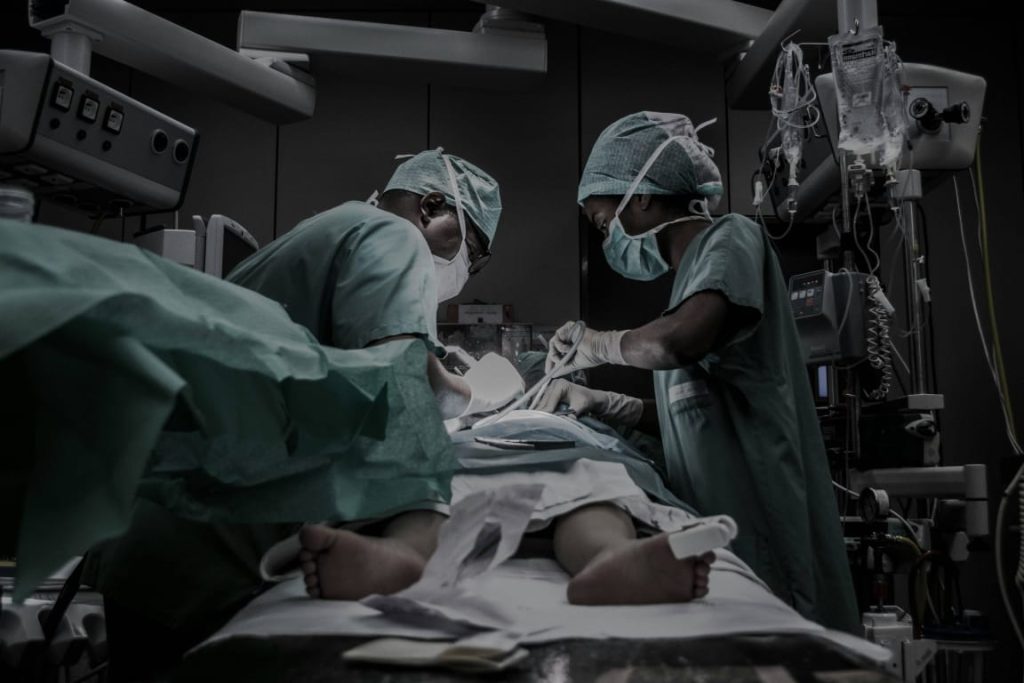
Nigerian healthcare workers often operate under difficult conditions
Opinion: Strengthening Collective Responsibility in Nigeria’s Health System
Nigeria’s healthcare system stands at a difficult crossroads. Recent developments show both hope and warning signs. Therefore, strengthening collective responsibility across government, professionals, and partners is no longer optional.
On one hand, collaboration between the Federal Government and humanitarian partners is expanding. On the other hand, medical professionals warn that the system faces deep structural risks. Consequently, the conversation about healthcare reform must move beyond isolated policy announcements.
A Health System Under Strain
Nigeria’s health sector has faced mounting pressure for years. However, recent warnings from medical professionals reveal how fragile the system has become.
Medical consultants recently warned that worsening brain drain could cripple healthcare delivery nationwide. They argued that the continued migration of doctors may push the system toward collapse if urgent reforms are not implemented.
Furthermore, many hospitals already struggle with staff shortages, outdated equipment, and poor infrastructure. As a result, healthcare workers often operate under difficult conditions. Consequently, morale continues to decline across the sector.
At the same time, migration among Nigerian professionals has grown steadily over the years. Skilled doctors and nurses often leave in search of better working conditions abroad. The challenge goes beyond workforce numbers. It now touches institutional stability, healthcare quality, and public trust.
Why Collective Responsibility Matters
Healthcare systems rarely collapse because of one problem alone. Instead, they weaken gradually when multiple responsibilities are neglected.
Government institutions must provide policy direction and adequate funding. Meanwhile, medical professionals must remain engaged in reform conversations. In addition, private sector actors and development partners must support innovation and capacity building.
Therefore, the idea of collective responsibility becomes central.
When different stakeholders work in isolation, progress slows dramatically. However, when collaboration becomes the norm, systemic change becomes possible.
Nigeria’s healthcare challenges illustrate this clearly. Infrastructure gaps persist partly because coordination among institutions remains inconsistent. Consequently, patients often experience fragmented care. Stronger collaboration could improve outcomes significantly.
Read More: Sterling Bank Backs Health, Tourism, and Creative Enterprise
Partnerships Offer a Path Forward
Recent developments show that collaboration can deliver meaningful progress. The Federal Government recently moved to deepen cooperation with Médecins Sans Frontières, also known as Doctors Without Borders. The discussions focused on strengthening humanitarian medical operations and addressing health system challenges.
Such partnerships matter because humanitarian organisations often fill critical gaps in underserved regions. Moreover, they bring technical expertise and operational experience that can strengthen national systems.
However, partnerships alone cannot solve structural weaknesses. They must therefore complement long-term investments in infrastructure, workforce training, and healthcare financing. Otherwise, short-term gains may disappear quickly.
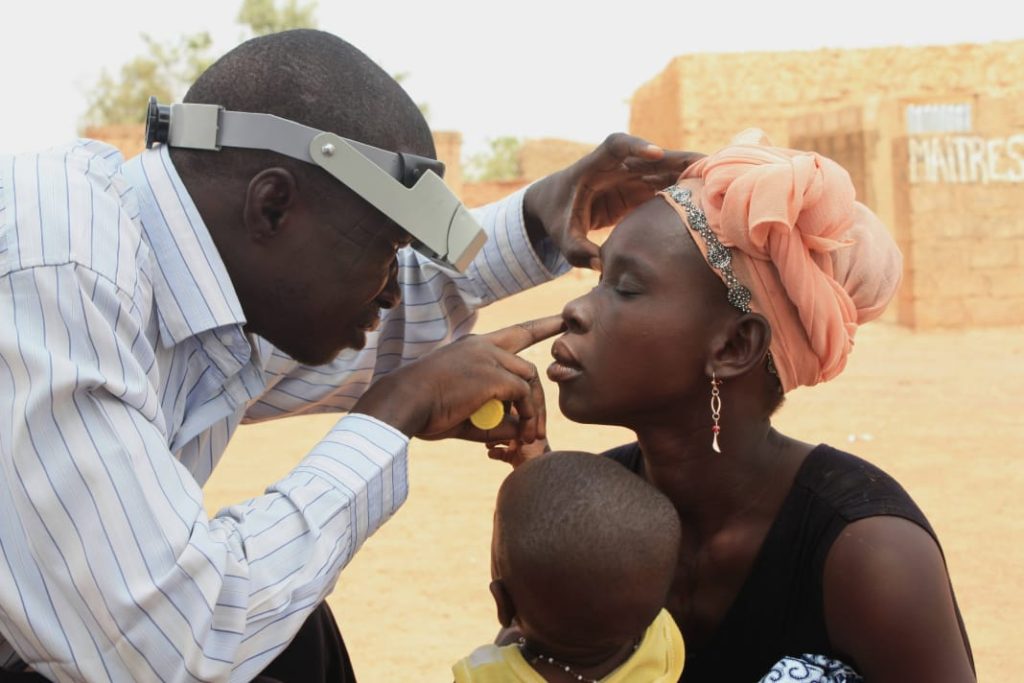
Retaining Talent Must Become a Priority
Nigeria cannot strengthen its health system without addressing the growing loss of medical professionals. Doctors often leave because of poor remuneration, heavy workloads, and limited professional opportunities. Consequently, hospitals struggle to maintain adequate staffing levels.
In addition, training institutions invest years preparing specialists who eventually leave the country. As a result, public resources effectively subsidize healthcare systems elsewhere. Therefore, retention strategies must become a national priority.
Improving working conditions represents an important first step. However, broader reforms must also address infrastructure, research opportunities, and career development. If professionals feel valued and supported, migration pressures may reduce.
Building a Sustainable Health Future
Collective responsibility should extend beyond government agencies and medical professionals. Private sector organisations, philanthropic foundations, and civil society groups also play important roles. Through investment and innovation, they can strengthen health services and expand access.
Furthermore, citizens themselves must remain engaged. Public demand for accountability often drives meaningful reform. However, sustained change requires long-term commitment from every stakeholder.
Nigeria’s health system will not improve overnight but coordinated action can gradually rebuild resilience. Therefore, the current moment should serve as both warning and opportunity.
If leaders strengthen partnerships, retain talent, and prioritise health investments, the system can recover. However, if collaboration fails, the warnings from medical experts may soon become reality. Ultimately, the future of healthcare in Nigeria depends on shared responsibility. And the time to strengthen that responsibility is now.
[give_form id="20698"]

