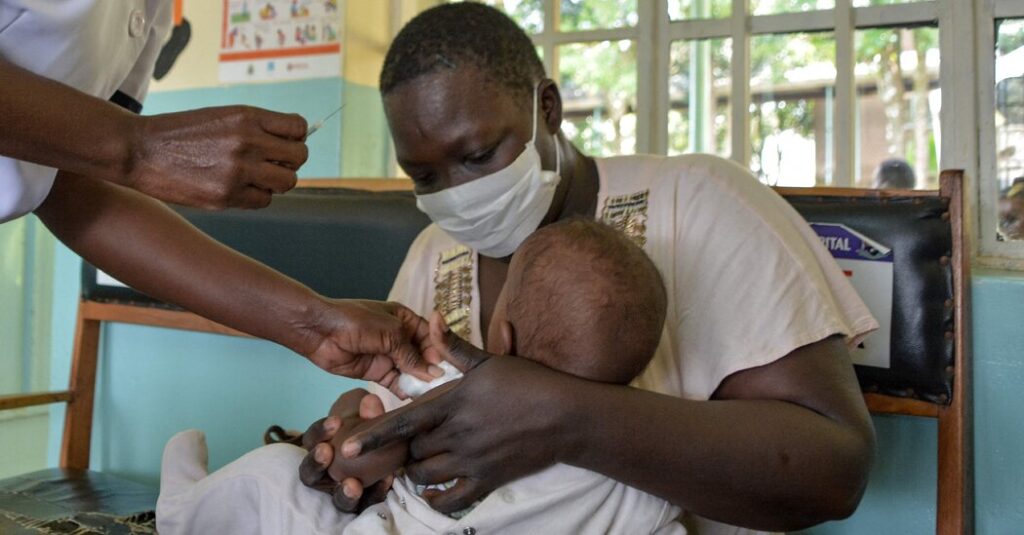
After years of steady gains in malaria prevention and treatment, progress has begun to stall. Infection rates are no longer declining at the pace once recorded. Funding gaps are widening. And the continent that carries the heaviest burden of the disease now faces a difficult reality: without sustainable financing, hard-won gains could unravel.
African leaders are increasingly raising the alarm.
The urgency is justified. According to the World Health Organization, Africa accounts for the vast majority of global malaria cases and deaths. While international funding mechanisms such as the Global Fund to Fight AIDS, Tuberculosis and Malaria have historically played a pivotal role in supporting national programmes, external financing is under strain amid competing global crises.
The funding model that once powered malaria reduction across the continent is no longer sufficient for the scale of the challenge ahead.
The Plateau After Progress
For nearly two decades, malaria mortality rates declined due to coordinated efforts in insecticide-treated bed nets, rapid diagnostic testing, artemisinin-based therapies, and expanded community health systems.
But momentum has slowed.
Population growth, climate variability, resistance to insecticides and antimalarial drugs, fragile health systems, and underfunded primary healthcare infrastructures are complicating the fight. In some high-burden countries, cases are rising again.
The stagnation is not simply a public health issue. It is an economic and development concern.
Malaria reduces workforce productivity, increases healthcare expenditure, disrupts schooling, and undermines economic resilience. For countries striving toward inclusive growth and poverty reduction, sustained malaria prevalence creates structural drag.
Why Financing Is the Critical Fault Line
The core issue is no longer only medical. It is financial.
Many African countries still rely heavily on donor funding for malaria prevention, testing, and treatment. As global development assistance faces pressure, domestic budget allocations have not increased at a pace sufficient to compensate.
Health financing remains constrained by debt servicing obligations, fiscal limitations, and competing national priorities. In this context, malaria programmes risk underfunding precisely when innovation and sustained intervention are most needed.
African leaders are therefore shifting the narrative — from donor dependency to sustainable, domestically anchored financing strategies.
This includes:
- Integrating malaria financing into national health insurance schemes
- Expanding private sector participation
- Strengthening domestic resource mobilisation
- Leveraging innovative financing mechanisms
The message is clear: external aid can complement, but it cannot substitute for sovereign commitment.
Climate Change and the Expanding Risk Map
Climate change adds another layer of urgency.
Rising temperatures, altered rainfall patterns, and flooding are expanding mosquito breeding environments into previously low-transmission zones. Urbanisation without adequate drainage infrastructure further compounds exposure risk.
Malaria control strategies must therefore evolve beyond traditional rural concentration models. Urban health systems, environmental planning, and climate adaptation frameworks must now intersect with malaria prevention.
This convergence demands coordinated financing — not fragmented interventions.
Private Sector and ESG Alignment
There is also an emerging opportunity within the corporate sector.
Companies operating in high-burden regions face productivity losses and community vulnerability linked to malaria prevalence. Structured malaria prevention programmes align directly with ESG commitments, particularly under the “S” pillar of social investment and community health.
Corporate co-financing models, workforce protection schemes, and public-private partnerships can strengthen resilience while advancing sustainability credibility.
The malaria fight, when viewed through an ESG lens, becomes not only a public health obligation but a strategic investment in human capital.
Beyond Emergency Response
One of the risks facing malaria control efforts is the tendency toward cyclical emergency responses. Funding surges during outbreaks, then declines when visibility fades.
Sustainable financing demands a shift from reactive models to predictable, multi-year budgeting anchored in national development strategies.
Health system strengthening must become central. Community health workers require stable remuneration. Supply chains for diagnostics and treatments must be resilient. Surveillance systems must be digitised and integrated.
Short-term grants cannot substitute for structural capacity.
A Continental Inflection Point
Africa stands at a crossroads.
The continent has demonstrated that malaria deaths can decline with coordinated intervention. The scientific tools exist. The community networks exist. The institutional knowledge exists.
What is at risk is continuity.
If funding stagnation persists, resistance patterns may worsen, prevention coverage may drop, and mortality could climb. The cost of reversal would exceed the cost of sustained investment.
African leaders calling for sustainable malaria financing are not merely advocating for more money. They are advocating for smarter, domestically embedded, accountable financing systems.
The Way Forward
Sustainable malaria financing requires a three-fold recalibration:
First, governments must prioritise health allocation within national budgets, recognising malaria control as an economic stabiliser, not simply a health line item.
Second, development partners must align financing with long-term capacity building rather than short-cycle project cycles.
Third, private sector actors must view malaria prevention as part of their social licence to operate in vulnerable communities.
Malaria elimination is not solely a medical ambition. It is a governance, financing, and accountability challenge.
A Test of Commitment
The slowdown in malaria progress is a warning — but not yet a reversal.
With strategic financing, coordinated leadership, and institutional accountability, Africa can regain momentum. Without it, the continent risks sliding backward after years of measurable progress.
The choice before policymakers is clear: treat malaria financing as a temporary burden, or as a long-term investment in economic resilience and human capital.
History has already shown what sustained funding can achieve.
The next chapter will reveal whether that commitment can be renewed — and strengthened.
[give_form id="20698"]

